What is Eczema – Atopic Dermatitis: Causes, Triggers, and Symptoms
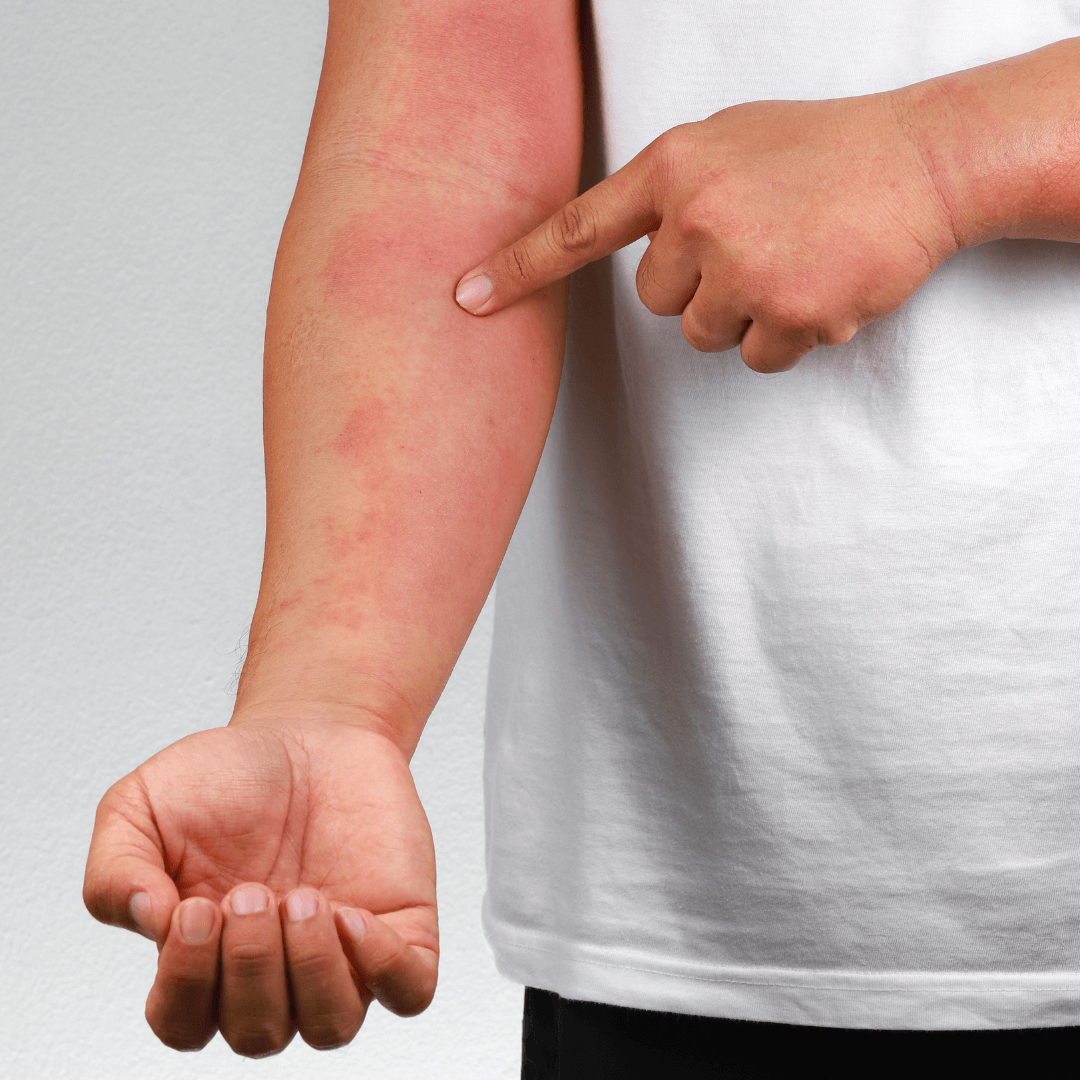
If your skin is dry, itchy, cracked, red and/or inflamed, you might have eczema (atopic dermatitis) Eczema is very normal, very common, and very, very uncomfortable. It can affect your quality of life and can keep you from sleeping, distract you and make you feel self-conscious in public. You are not alone! 15% to 20% of people experience eczema or another type of dermatitis at some point in their lives.
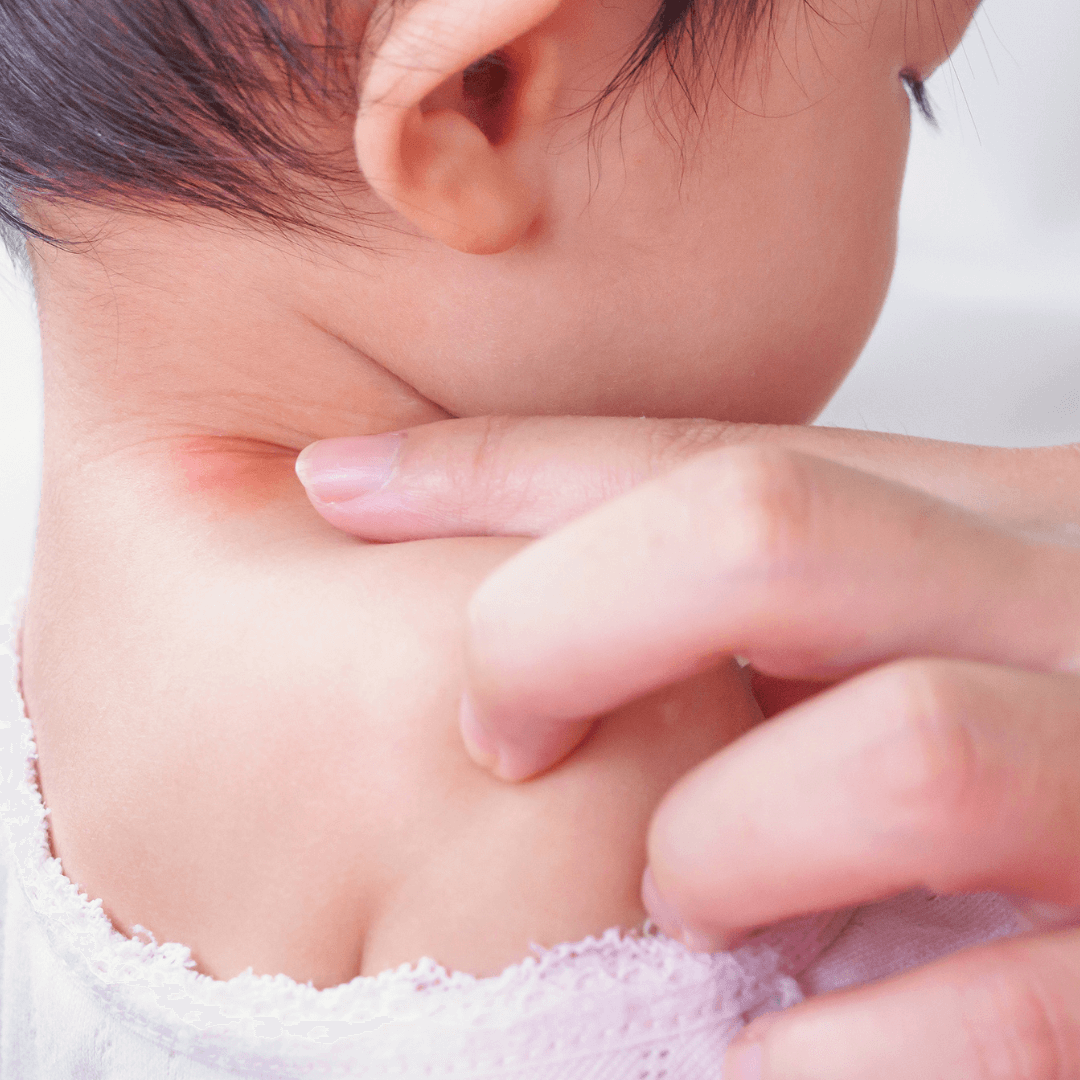
Atopic eczema is more common in children, often developing before their first birthday. But it may also develop for the first time in adults. It’s usually a long-term (chronic) condition, although it can improve significantly, or even clear completely in some children as they get older.
Symptoms of atopic eczema
Atopic eczema causes the skin to become itchy, dry, cracked and sore. Some people only have small patches of dry skin, but others may experience widespread inflamed skin all over the body. Symptoms could be keeping you awake at night, making it hard to complete daily tasks, skin is peeling, prickling, blistering or weeping fluids or getting thick and scaly.
Inflamed skin can become red on lighter skin, and darker brown, purple or grey on darker skin. This can also be more difficult to see on darker skin.
Although atopic eczema can affect any part of the body, it most often affects the hands, insides of the elbows, backs of the knees and the face and scalp in children.
People with atopic eczema usually have periods when symptoms are less noticeable, as well as periods when symptoms become more severe (flare-ups).
When to seek medical advice
See your health provider if you have symptoms of atopic eczema. They’ll usually be able to diagnose atopic eczema by looking at your skin and asking questions, such as:
- whether the rash is itchy and where it appears
- when the symptoms first began
- whether it comes and goes over time
- whether there’s a history of atopic eczema in your family
- whether you have any other conditions, such as asthma or allergies
- whether something in your diet or lifestyle may be contributing to your symptoms
What questions should I ask my healthcare provider about eczema (atopic dermatitis)?
- How can you tell that I have eczema?
- If I don’t have eczema, what other skin condition might I have?
- Is there a specific brand of moisturizer that you recommend?
- Is there a prescription cream that you can prescribe?
- How often should I see a dermatologist regarding my eczema?
- What soaps, lotions, makeup, etc. should I avoid?
- What medications do you recommend?
- What at-home treatments do you recommend?
Typically, to be diagnosed with atopic eczema you should have had an itchy skin condition in the last 12 months and 3 or more of the following:
- visibly irritated red skin in the creases of your skin – such as the insides of your elbows or behind your knees (or on the cheeks, outsides of elbows, or fronts of the knees in children aged 18 months or under) at the time of examination by a health professional
- a history of skin irritation occurring in the same areas mentioned above
- generally dry skin in the last 12 months
- a history of hay fever or asthma – children under 4 must have an immediate relative, such as a parent, brother or sister, who has 1 of these conditions
- the condition started before the age of 2 (this does not apply to children under the age of 4)
Causes of atopic eczema
Eczema (atopic dermatitis) is caused by a combination of immune system activation, genetics, environmental triggers and stress.
- Your immune system. If you have eczema, your immune system overreacts to small irritants or allergens (“atopic means sensitivity to allergens”) . This overreaction can inflame your skin.
- Your genetics. You’re more likely to have eczema if there is a history of dermatitis in your family. You’re also at a higher risk if there’s a history of asthma, allergens and/or hay fever. Allergens are substances like pollen, pet hair or foods that trigger an allergic reaction. Also, there might be a change in your genes that control a protein that helps your body maintain healthy skin. Without normal levels of that protein, your skin will not be completely healthy.
- Your environment. There is a lot in your environment that can irritate your skin. Some examples include exposure to tobacco smoke, air pollutants, harsh soaps and detergents, fabrics such as wool and some skin products. Low humidity (dry air) can cause your skin to become dry and itchy. Heat and high humidity can cause sweating and that can make the itchiness even worse.
- Your stress. Your stress levels can cause or worsen your eczema. There are mental/emotional signs of stress and physical signs of stress
Allergy tests are not usually needed, although they’re sometimes helpful in identifying whether a food allergy may be triggering symptoms.
Treating atopic eczema
Treatment for atopic eczema can help to relieve the symptoms and many cases improve over time.
But there’s currently no cure and severe eczema often has a significant impact on daily life, which may be difficult to cope with physically and mentally.
There’s also an increased risk of skin infections.
Many different treatments can be used to control symptoms and manage eczema, including:
- Self-care techniques, such as reducing scratching and avoiding triggers
- Emollient (moisturizing creams or treatments) – used on a daily basis fo
- topical corticosteroids – used to reduce swelling, redness and itching during flare-ups
How do I take care of myself?
Reducing your stress is very important. Try these tips:
- Count to ten as you take a deep breath.
- Exercise daily.
- Try not to drink as much caffeine and alcohol.
- Sleep eight hours a night.
- Eat healthy.
- Try to have a positive attitude.
- Journal every day.
- Talk about your life with friends, family and a therapist.
Other types of eczema
Eczema is the name for a group of skin conditions that cause dry, irritated skin.
Other types of eczema include:
- discoid eczema – a type of eczema that occurs in circular or oval patches on the skin
- contact dermatitis – a type of eczema that occurs when the body comes into contact with a particular substance
- dyshidrotic eczema (pompholyx) – a type of eczema that causes tiny blisters to erupt across the palms of the hands
- varicose eczema – a type of eczema that most often affects the lower legs and is caused by problems with the flow of blood through the leg veins
- sebhorrhoeic eczema– a type of eczema where red, scaly patches develop on the sides of the nose, eyebrows, ears and scalp
Living with eczema can be challenging. There may be times when your eczema disappears. This is known as a “remission” period. Other times you may have a “flare-up,” which is when it gets worse. The goal of treatment is to prevent such flare-ups, preventing your symptoms from getting worse. Be sure to avoid triggers, moisturize with George’s Special Dry Skin Cream (recommended by physicians, pharmacists and dermatologists) to calm, soothe and hydrate your skin, take your medicine and do anything else your healthcare provider recommends.
THIS CONTENT DOES NOT PROVIDE MEDICAL ADVICE. This website serves the purpose of providing general information and does not in any way replace or substitute professional medical advice, diagnosis or treatment. Always seek the advice of a qualified healthcare professional regarding your health. If you think you may have a medical emergency, contact your doctor immediately or call 911.